Back in 2013, ComplianceBug found approximately 32% of health and welfare plans penalized since 2000 were in excess of $10,000 after examining the Department of Labor’s (DOL’s) Employee Benefits Security Administration (EBSA) database that tracks enforcement efforts on deficient filers, late filers and non-filers of annual Form 5500’s.
“Since it’s been more than a decade since we last reviewed the data, we wanted to see if the ‘tools and resources’ that are typically provided by insurance brokers and consultants were effective in assisting their employer clients with compliance efforts,” said Peter Lewenson, founder and President of ComplianceBug.
The EBSA’s latest dataset was published on January 3, 2025 and now contains 25 years worth (2000-2024) of closed cases that resulted in penalty assessments.
ComplianceBug now finds approximately 36% of the health and welfare plans penalized over last 10 years (2015-2024) were in excess of $10,000 and 7% in excess of $50,000. This represents an increase over the 2000-2012 enforcement data.
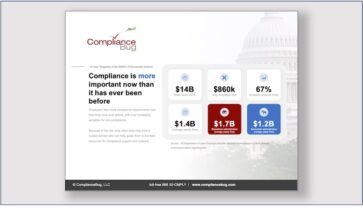
DOL EBSA Enforcement
“It’s not surprising,” continues Lewenson. “Every day we talk to non-compliant employers who were never told their group benefits needed to comply with ERISA law or they were provided wrong materials by their broker consultants. This leads to never filing, or incorrectly filing, wrong 5500’s. It’s often just the tip of the iceberg of issues we find when conducting a compliance risk analysis.”
Furthermore, the data appears to coincide with other enforcement actions. In fiscal year 2024, the EBSA received a total of 199,094 compliants from participants and beneficiaries via their Informal Compliant Resolution program. These informal complaints along with other EBSA initiatives led to investigations where more than 71% of audited plans were found to be non-compliant. As a result, a total of $1.4 billion in fines, penalties and plan restitutions were collected (averaging $2.7 million per investigation).
What should you do
Don’t get caught off guard. Don’t assume new political administrations will conduct less enforcement. During the last Trump administration, the EBSA’s enforcement actions were actually 81% higher 2017-2020 ($6.8 billion) vs. Obama’s 2013-2016 ($3.7 billion) administration.
Employers are urged to require their insurance broker/agent, carrier/TPA, or other group benefit consultant to provide the necessary tools to measure, illustrate and monitor compliance risk.
Knowing your organization’s compliance risk via a proactive compliance assessment and then tracking on-going compliance efforts is the best way to prepare for and ensure when the DOL’s EBSA requests an audit, your health & welfare benefit plans are compliant.