Pretty much every day we get asked the same question: Does anyone really enforce non-compliance?
The short answer is, yes. And it’s actually more of a possibility than you might believe. Each day, both the IRS and DOL (Department of Labor) send “notices of intent to assess a penalty” to employers. Depending on what deficiency they have discovered, the penalty amounts can be staggering.
The IRS and DOL have agreements to work together
Various government agencies share data to enforce compliance for employee benefits and many other things. For example, the DOL, IRS, and Pension Benefit Guaranty Corporation (PBGC) jointly release and process Form 5500 data for retirement and welfare plans.
But there exist even more specialized, formal agreements known as Memorandum of Understanding (MOU’s) between various divisions within these agencies. These agreements facilitate information sharing, joint investigations, and referrals to combat non-compliance.
One MOU signed in June 2023 between the Internal Revenue Service’s Tax-Exempt and Government Entities Division (TEGE) and the Department of Labor’s Employee Benefits Security Administration (EBSA) reflects changes resulting from the implementation of the IRS FTI Secure Data Transfer (SDT) Tool and other revisions identified from the agencies’ experiences under prior agreements. (PDF of MOU) (link to DOL) (HTML version)
Note that the TEGE division of the IRS is a bit of a misnomer. While the division’s name has the words “tax-exempt” and “government entities” in it, that is not all that it does.
Within the guidance provided by the DOL in the signed MOU, while their focus is on retirement and related plans, the formal MOU specifically spells out what to do with welfare plans:
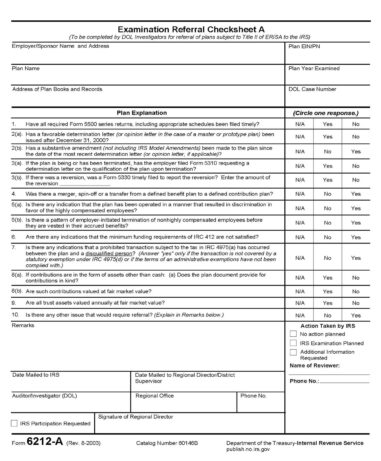
“DOL will continue to refer Form 6212-A to IRS for welfare benefit plans and pension benefit plans in accordance with the requirements of Article II, D., of the Agreement. IRS will continue to make referrals to DOL on Form 6212-B in accordance with the requirements of Article II, C. of the Agreement.“
What is Form 6212?
Form 6212 is an internal government form that has two versions which differ based on which agency is completing the form.
- The DOL uses Form 6212-A to refer plans to the IRS for further investigation.
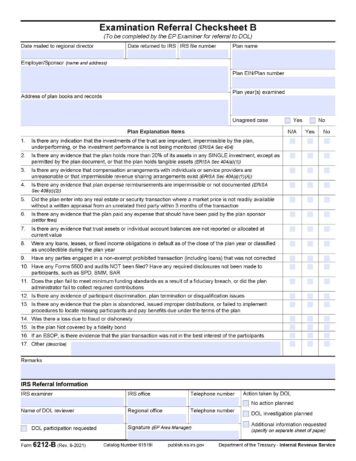
- The IRS uses Form 6212-B to make referrals to the DOL for further investigation.
Based on automated internal systems and, possibly, programs like the Informal Compliant Resolution program, auditors/investigators use these forms to flag plans for possible “red-flags” and further investigation by the other department.
How could a referral be used against a health & welfare plan?
We think for group health and welfare benefits, the IRS’s Form 6212-B (used to ask the DOL for further investigation) is interesting for this question:
- (10) Have any Form 5500 and audits NOT been filed? Have any required disclosures not been made to participants, such as SPD, SMM, SAR
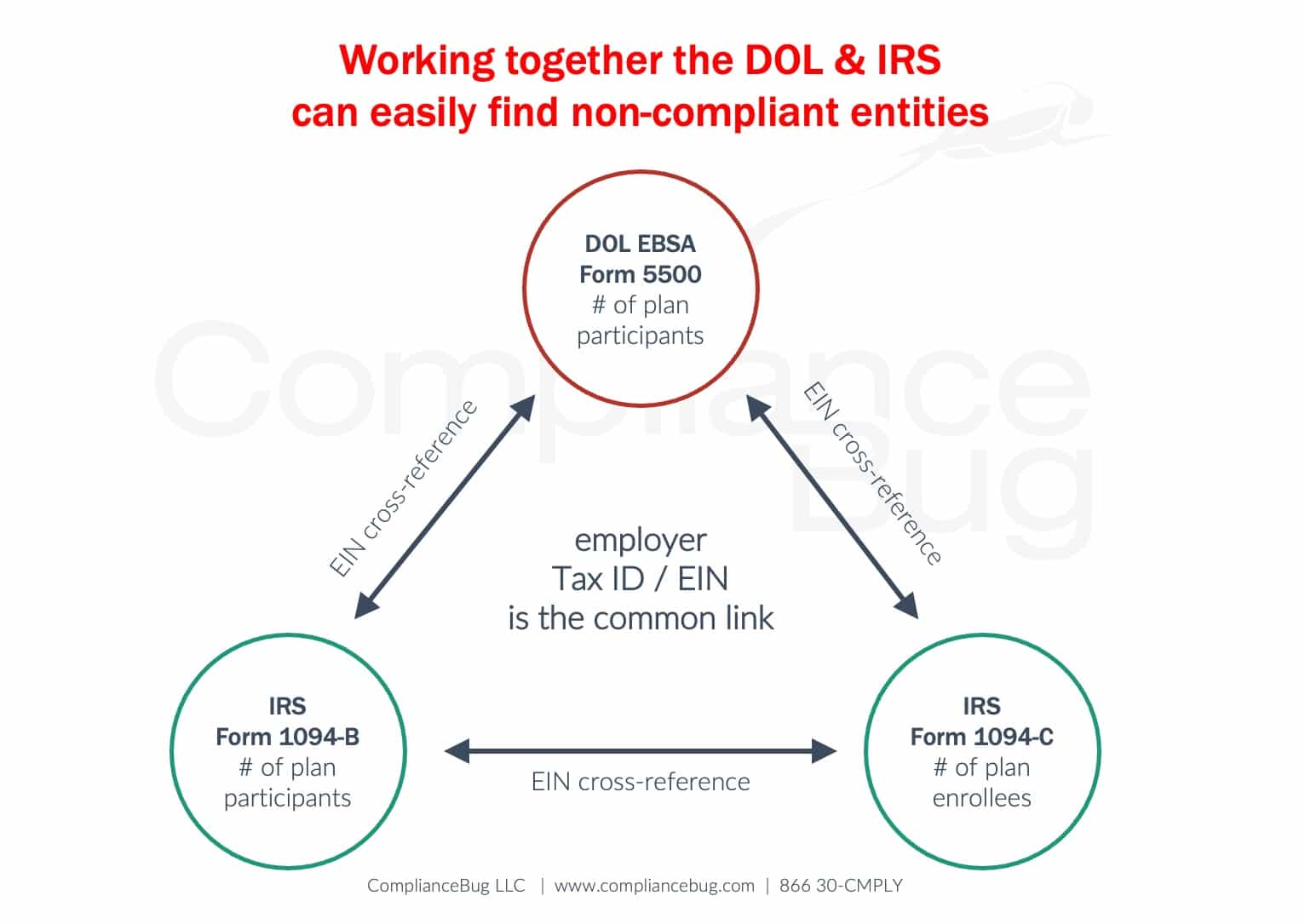
Under the Affordable Care Act, when the IRS receives Forms 1094-B and 1094-C from insurers and applicable large employers (ALE’s) to summarize the total number individuals with minimum essential coverage, the IRS can easily identify health plans with more than 100 participants.
As we know, if a plan has more than 100 participants at the beginning of their plan year, it’s required to file a Form 5500. If the IRS cannot find a Form 5500 for that plan using the EIN on the Form 1094, it’s quite easy to then refer them to the DOL as a non-compliant plan.
At the time we’re publishing this, failure to file a Form 5500 can result in penalties from the DOL of $2,739 per day with no limit and $250 per day by the IRS (up to $150,000 per plan) for each annual report not filed.
We believe, in a similar fashion, the DOL could use Form 5500 retirement plan data to report back to the IRS plans with more than 50 employees to identify possible employers with delinquent Form 1095’s.
So what can you do
Require your insurance broker/agent, carrier/TPA, or other group benefit consultant to provide the necessary compliance tools to measure, illustrate and monitor compliance risk.
Knowing your organization’s compliance risk via a proactive compliance assessment and then tracking on-going compliance efforts is the best way to validate your health & welfare benefit plans are compliant.






