As employers struggle to keep up with the regulatory changes that impact their group health plans, many turn to their group benefits insurance broker for help with ACA, ERISA, COBRA and HIPAA compliance requirements.
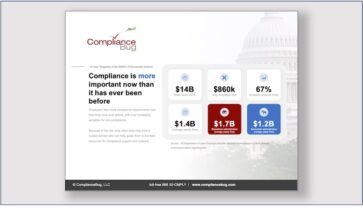
However, relying on only your broker can put you and your benefit plans at risk for significant fines, penalties & lawsuits. Just last year, the Department of Labor (DOL) collected more than $1.2 billion in compliance penalties and has now increased their enforcement efforts by hiring additional investigators and auditors with a $141 million budget for 2013.
The last thing your broker wants to do is give you a headache. While insurance brokers are required to be licensed in the state in which they sell and mange insurance policies, there aren’t any requirements for them to know the details about the federal, state and local laws that govern group benefit plans.
In their desire to provide value to clients, a broker might overstate their true expertise. Or they might rely on a 3rd party vendor and say they will protect you – but, if you review a contract, it typically limits their liability and may not provide you any indemnification even if a mistake is made.
To help employers avoid ERISA violations, we put together 4 common mistakes brokers make with their clients. Take a minute to review the following list to see how they apply to you and your benefit plans. If any one of these issues applies to you, strongly consider performing a self-audit of your plans to ensure they are in compliance with applicable laws.
4 Ways Your Benefits Broker Puts You at Risk for ERISA Violations
1. Not reviewing ERISA Plan Documents / Summary Plan Descriptions (SPDs)
With limited exceptions for public sector and church plans, ERISA requires all group benefit plans (no matter the number of employees) to have an up-to-date ERISA Plan Document and SPD. However, when renewing coverage, if the benefits, eligibility and other definitions aren’t consistent between the insurance policy and these documents, participants can sue to recover benefits they believe they were entitled to. Learn how to protect yourself from group benefit compliance risk.
2. Indicating your carrier documents satisfy ERISA requirements
It’s all too easy to confuse the tons of official looking carrier paperwork and contracts with an actual ERISA SPD. All too often, brokers incorrectly tell their clients the carrier’s “benefits summary” guides are the “ERISA SPD”. It’s rare that a carrier would produce an SPD. If you check the fine print of the carrier’s summaries you’ll typically see it says “…this is NOT to be considered an official SPD under ERISA. Please check with your plan sponsor/administrator for the actual ERISA SPD.” If you thought your broker handled #1 above, you might want to think again… Department of Labor fines and penalties accrue at $110 per day per covered employee for failing to provide a participant with an SPD.
3. Telling you your voluntary/worksite benefits are ERISA exempt
A cost effective way for an employer to offer additional benefits to employees is via voluntary or worksite benefits. Brokers often entice employers to offer these benefits by providing the employer enrollment systems or conducting educational seminars for employees. Depending on how the employer conducts themselves with the setup and maintenance of these benefits, the benefits could be subject to ERISA violations if they fail the voluntary benefit plan safe harbor rules. Non-compliance with ERISA can lead to fines and penalties between $110 to (in some cases) $1,100 per day along with potential lawsuits from current and former employees.
4. Changing your renewal date
As a way to push back the need to comply with Health Care Reform provisions or to negotiate lower insurance premiums, changing your renewal date is not a simple task. Performing this change impacts COBRA administration, Section 125 cafeteria plans rules, FSAs, HRAs, Form 5500 deadlines, employee notice requirements and many other things. Just asking the carrier to change their policy date can have far reaching consequences and compliance pitfalls. And that’s if you want to shorten your plan year to less than 12 months. If, in previous years, you pushed back annual enrollment and got an “extension” to 13 months (or more) definitely puts you out of compliance under IRS guidelines and subjects you to possible excise taxes and plan disqualification.
Conclusions
As the DOL, IRS and Health & Human Services (HHS) have increased their compliance enforcement for group health & welfare plans, it’s important for employers to take control of their plan responsibilities and partner with insurance brokers who proactively identify compliance issues and not just provide passive solutions.
Have you performed an annual compliance risk assessment?
Is it something you’re considering? Share your thoughts with us!